While the intent of nerve imaging (the ‘why’) is imperative to determining the optimal imaging method, general characteristics of nerve imaging technology include:
- Superb contrast of the nerve relative to its background (i.e., signal-to-noise ratio) to discern the functional status of axons thereby facilitating better injury diagnosis and detailed monitoring.
- Diagnose injuries and diseases of the peripheral nervous system
- Track regeneration/healing.
- 3D rendering of nerve anatomy.
- High reproducibility and minimizing user variation
- Readily accessible
- Cost and time effective
- Real-time use
Magnetic Resonance Imaging (MRI)
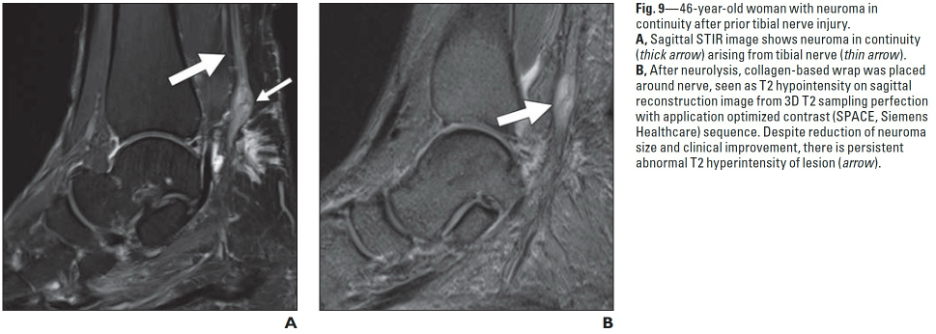
MRI works by using a magnetic to ‘excite’ protons (hydrogen atoms) within tissue and recording how they ‘relax’ which provides a signature of the tissue and tissue state. MRI-based techniques, including diffusion-weighted imaging, diffusion tensor imaging and microneurography, have shown significant potential for clinically relevant anatomical imaging of peripheral nerves1, including diagnosis of peripheral nerve injury2 and 3D rendering.
Drawbacks to MRI neurography include:
- Limited availability of suitable MRI machines
- Cost of suitable MRI
- Time required to obtain the image
- Motion artifact which is a blurring of the image if the patient is not (absolutely) still during the MRI.
- Need for sedation (anesthesia) at times to keep patients still
Ultrasound
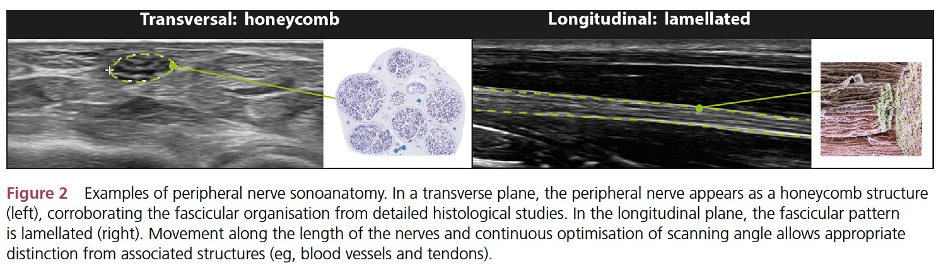
Ultrasound is also considered one of the safest forms of internal imaging because it does not use electromagnetic radiation or ionizing radiation (e.g., x-ray). As with other imaging modalities, a detailed knowledge of anatomical landmarks is necessary for this technique and therefore demonstrates user variation. Ultrasound can be used to identify and localize alterations in nerve continuity. Therefore, it can be useful in estimating nerve injury in a granular manner, as a visual guide for invasive procedures and intra-operative exploration, and to diagnose postoperative nerve repair complications4 such as neuromas. In addition, because it is real-time, ultrasound is used to provide visual guidance for delicate tasks such as injections (e.g., steroid) around nerves5
Disadvantages of ultrasound include:
- Visualization is limited to superficial nerves
- Poor contrast with increasing depth
- Lower contrast resolution than MRI
- Unable to distinguish subfascicular details of regeneration such as axonal regrowth or distinguish absent or nonfunctional axons from functional axons.
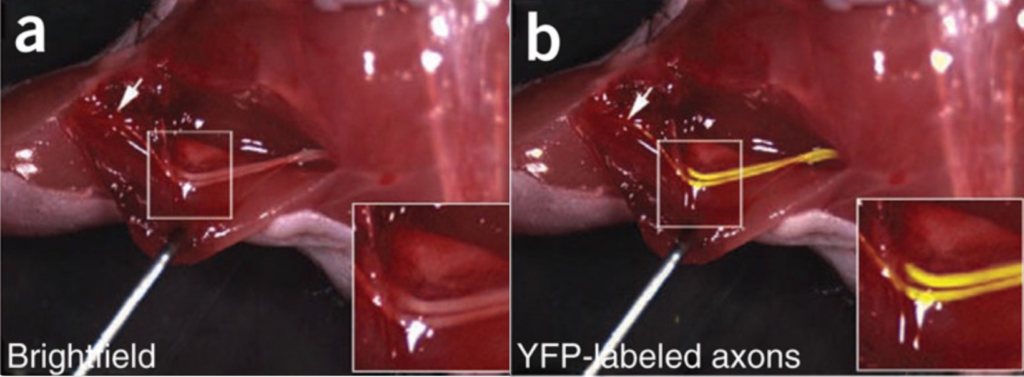
Fluorescent-Guided Surgery
This technology uses the building blocks of proteins, called peptides, that are labeled with fluorescein, a dye that appears bright under specific lighting. This composite of peptide + fluorescein then binds to nerves after being injected intravenously and is subsequently imaged using a microscope. Several of these are in various stages of clinical development 7. Favorable attributes to this approach are high contrast within the nerve, real-time capability to protect nerves, and 3D rendering. Preliminary disadvantages include the need to make an incision to use the technology, need for proprietary microscope, limited depth of visualization.